Silent Virus Linked to Severe Brain Disease in Adults
A little-known virus may infect most people, but new research reveals a potential link to brain disease in those with chronic kidney issues. Vigilance is essential as cases rise.
A previously obscure virus is believed to infect up to 90 percent of individuals and remains dormant in their cells for life. However, if activated, it can lead to severe brain damage. Recent research indicates a possible new trigger for this virus, impacting up to 10 percent of adults globally.
The virus, known as human polyomavirus 2, or the JC virus, is named after the patient from whom it was first isolated in 1971. It is present in the urine and stool of infected individuals and spreads through the fecal-oral route. Many people are thought to contract the virus early in life, with blood tests suggesting that 50 to 90 percent of adults have been exposed at some point.
Researchers believe that the tonsils or gastrointestinal tract may serve as the initial infection site, although this early infection typically remains asymptomatic. During this phase, individuals carry what is termed the archetype JC virus, which establishes a silent, lifelong infection.
For most people, the JC virus infection remains symptomless. However, in certain cases, the virus can reactivate, altering its genetic structure and transforming into a variant that causes a life-threatening condition known as progressive multifocal leukoencephalopathy (PML).
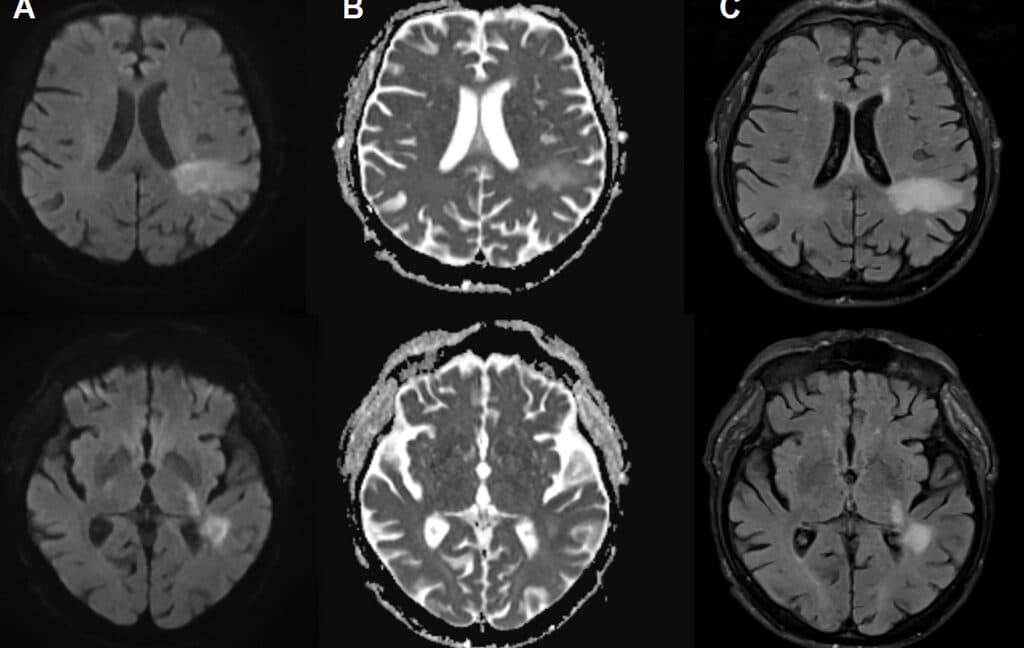
PML occurs when the modified JC virus infiltrates the brain, damaging specific brain cells, including those responsible for creating myelin sheaths that protect nerve cells. This results in significant demyelination, leading to nerve cell dysfunction and death. Diagnosing PML typically involves identifying distinctive brain lesions through imaging and detecting JC virus DNA in cerebrospinal fluid. Symptoms of PML can resemble those of a stroke or multiple sclerosis, including speech and visual impairments, motor dysfunction, and seizures.
PML was first documented in 1958 in a cancer patient but was considered rare until the 1980s when it began appearing in patients with HIV/AIDS. During the early epidemic, PML became an AIDS-defining illness, affecting 2 to 5 percent of HIV-positive individuals. At that time, the condition was often fatal. However, following the introduction of highly active antiretroviral therapy (HAART) in 1996, PML cases declined, and survival rates improved, although many survivors experience lasting damage.
Historically, PML has been associated with severe immune suppression. It is believed that the JC virus can only become a PML-type virus in the absence of adequate immune defense. The restoration of immune function, such as through HAART in HIV patients, can help prevent or manage PML. In addition to HIV/AIDS and certain cancers, PML may also occur in patients taking powerful immunosuppressive medications for conditions like multiple sclerosis or autoimmune diseases. Overall, PML is estimated to affect about 2 in 100,000 individuals worldwide.
Recently, a case study published in the Annals of Internal Medicine reported a PML case in a patient without significant immune suppression. Instead, the individual had chronic kidney disease (CKD), affecting approximately 10 percent of adults globally. CKD can lead to toxin accumulation in the bloodstream, impairing immune responses and increasing inflammation, which may reduce the body's ability to combat viral infections.
The patient, a 72-year-old man with stage-5 CKD, sought hospital care for neurological issues. He had been experiencing difficulty with word recall, confusion, and general weakness. Hospital tests confirmed his speech difficulties, prompting further evaluation.
Initially, doctors suspected uremic encephalopathy—a decline in brain function due to toxin buildup from kidney failure. Although treated with dialysis, the patient's condition deteriorated, leading to brain imaging that revealed lesions associated with PML. Subsequent tests confirmed the presence of the JC virus in his cerebrospinal fluid, and the patient passed away two days later.
While limited, existing literature has noted other PML cases in individuals with CKD. The authors of this study concluded that CKD adds to the range of conditions that may predispose individuals to PML through atypical immunosuppression. As the prevalence of CKD continues to rise globally, increased awareness of this serious complication is crucial.
